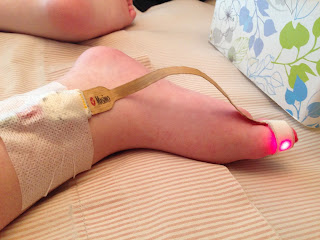
Ellie uses a continuous monitoring pulse ox during the night and when she is sick. There have been nights when we stumble out of bed because of incessant beeping and we are madly increasing oxygen, suctioning, rubbing her chest, etc to get her to breathe and get her sats up. Then we realize...the pulse ox is not attached and yes, the carpet's oxygen is maintaining a steady 68. Ha ha.
To resolve this problem we tape the pulse ox probe in place. We have found that if we leave a little bump in the probe wires (not pulling it tight against her skin) it stays on better and the probes don't wear out as fast.
We prefer the non-sticky probes (we like the velcro kind) they seen to last A LOT longer. Ellie does not move a lot, but our probes last anywhere from 1-3 months. I think the more your child moves the faster they wear out.
We use mefix. Ellie is really sensitive to adhesives, but the mefix does not bother her at all. I cut up a whole roll at a time and have a little stack of pre-cut mefix ready to go. There are even lines on the mefix that I cut on that make it the perfect length for this purpose.
On a slightly different note. I was told when she was little that red fingernail or toenail polish could affect the pulse ox reading. I have never found this to be the case.
How do you keep your pulse ox probe in place? What tips do you have for getting an accurate reading? Please "like" our FB page for more posts about raising a child with severe disabilities. https://www.facebook.com/SupportedInOurTrials/?ref=aymt_homepage_panel
background
Friday, August 5, 2016
Sunday, July 31, 2016
Packing list
Do you ever take your child with special needs on vacation or camping? It is a TON TON TON of work.
Ellie uses bipap, oxygen, suction, pulse ox, feeding pump, is cathed, uses a wheelchair, and on and on. Trust me...I know how difficult it can be. Not only is it hard physically, but I have a hard time committing emotionally. I have had multiple occasions where vacations have been changed, delayed or cancelled completely due to changes in medical status.
One thing I have done to lighten my load slightly is to have a packing list saved on my computer to pack for Ellie to go on vacation. Iwrote it as a camping list, but it is virtually the same list to go to a hotel...but we can leave off the generator and a few other things.
Some of the things I'm sure only make sense to me...so feel free to ask questions of how we do it, why we do it, why we take certain items etc.
I have found over the last few years that it is easier to pack Ellie's things in the same size of clear bins. You can see what is inside, group like things and they stack nicely in the car and in the hotel room.
I put each container on a separate sheet of paper on the list to clarify what fits and goes inside of each bin. I like to group like things such as her nebulizer items go together and her clothes go together.
Her "emergency med bag" is her emergency meds that are always on her wheelchair.
Her "med go bag" is a large cosmetic bag I keep stocked with syringes, water, pill crushers, etc. In one pocket and an empty pocket that I can shove all her meds into if I need to grab them and go somewhere.
Box 1 is formula supplies
Box 2 is Breathing (nebulizer, suction, oxygen) and Hygiene
Box 3 is Cathing and Sanitizing/Cleaning
Here is a link to Ellie's packing list that you can look at as an example. This list would obviously be different for your own medical needs and circumstances,
What tips and tricks do you have for packing to go on vacation or camping? Please share with us below. Please visit our FB page and like it to see future posts like this one.
Friday, May 27, 2016
Instant Info About Meds
There are some things you can know about meds instantly that you may not have realized.
For liquid meds...
If it is transparent (you can see through the liquid) you do not need to shake it.
If it is opaque (you CANNOT see through it) you will need to shake it first.
For ampules (for nebulizer)...
If they come in a foil pouch, then you will need to protect them from light.
It they come in the box (but no foil pouch), then there is NO NEED to protect them from light.
Do you have any other "Instant Info About Meds" you can share with us?
Please like our FB page. https://www.facebook.com/SupportedInOurTrials/
Thursday, May 26, 2016
Sleeping with eyes open or using cpap
Since this blog is about lessons I have learned...some things I have to confess I am kind of embarrassed about. But I am hoping by sharing that you won't have to learn the same lessons I did.
My daughter has always slept with her eyes partially open. In addition to that she has also used bi-pap for 13 years.
I didn't think sleeping with your eyes open was a big deal, and for a typically developing person, it probably isn't. For non-medically complex people they still rub their eyes and can tell if their eyes feel really dry they would complain about it. With Ellie, this is not the case. She cannot bring her hands to her face and is non-verbal.
At her most recent eye exam the opthalmologist said that she had permanent scar tissue on her iris (colored part of her eye). She asked if she slept with her eyes open, I said yes. She said the scar tissue was caused by this. She said she should be okay, but if the scar tissue extended into her pupil (black part of eye) she would have vision loss in that area. That's all we need...more vision loss (insert sarcasm)!
The eye Dr. said we needed to get "eye gel for SEVERE dry eyes". The brand pictured above is what we have been using. We just squeeze a little into each eyes before bed. It is available over-the-counter. I believe it was around $10 for a tube?!?!?!
I wish we would have been warned before so we could have avoided eye damage...but that is life with a medically complex child. Consider yourself warned.
Does your child sleep with their eyes open? Do you have any experiences you can share with us? We would love to hear from you!
Please sign up on the right to receive posts by email, or "like" our FB page to see future posts.
https://www.facebook.com/SupportedInOurTrials/?ref=aymt_homepage_panel
Monday, May 23, 2016
Paying for a wheelchair modified van/lift/ramp
(These resources are for Utah)
Rebates from Car Manufacturers on a new vehicle
If you buy a new vehicle from the dealer and modify it, a lot of dealers will give you a rebate. Here are a few examples. https://www.ride-away.com/manufacturer-mobility-rebate-programs/
Assistive Technology Foundation (Zions Bank Low interest loan)
1-800-524-5152
http://www.uatpat.org/
Here is another link to the same program http://www.uatf.org/financing/
You turn in the application and they help you get a low interest loan through Zions bank. The loan will be 1/2 of prime and the Foundation pays the other half of the interest. They will help pay for a vehicle and/or modifications. The vehicle does not need to have the lift/ramp already installed. For loans over $10,000 you can usually get a 5 year term. It takes about 1 week for the loan to go through once all of the paperwork has been submitted. Once the application is complete it is good for 90 days (you have 90 days to find a vehicle). You can use the loan more than once.
Independent Living Centers (locations throughout Utah...each county has a designated one)
http://www.usor.utah.gov/division-of-rehabilitation-services/vocational-rehabilitation/independent-living-il/centers-for-independent-living
They will pay to modify a van with lift/ramp/tie downs/etc. They will not pay for the van itself. They will only do modifications on a van that is 1 year old or less. They have a long waiting list. They get money each July, but you will need to apply well before that.
Angels Hands
https://angelshands.org/
It sounds like they may help with the purchase of the actual vehicle.
I sent the following question to Angel's Hands...
Do you help pay for a wheelchair modified vehicle?
This is the response I received...
Thanks you for your inquiry. Angel’s Hands Foundation’s mission is to improve the quality of life for individuals with rare or undiagnosed diseases. If you believe you fit into that mission, the following steps are required:
1. The family must register with Angel’s Hands by completing the online ‘Registration Form’ under the AHF Forms tab.
2. A request for assistance must be submitted by completing the online ‘Assistance Request Form’ under the AHF Forms tab.
a. Proper documentation must be attached to the form or mailed within 30 days of request.
The request will be screened and submitted to the board for consideration.
Thanks,
Dennis
Helps pay for modifying vans. Does not often pay for the van itself. Has certain requirements that the van must meet such as..vehicle must be the current body style and under 50,000 miles. Rear entry is available up to 80,000 for some vehicles.Has an open application period. In 2019 it will
open Nov 1, 2019. https://steelmanfamilyfoundation.org
Contact your local Eagles/VFW/ Elks/Lions/ etc... They are often looking for a good fundraising idea.
Create a GoFundMe account and'or have fundraisers to help raise money.
If you are on the DSPD waiver, they will pay to modify a van with lift/ramp/tie downs/etc. They will not pay for the van itself. It takes several months to go through the approval process.
Karl Malone Foundation has purchased vehicles before.
(this may be an inactive non-profit...it was difficult to track down online)
Karl Malone Foundation for Kids
Po Box 429
Bountiful, UT 84011
How have you been able to pay for a wheelchair modified vehicle? Do you know of any other resources? Please comment below.
You can also like my FB page to get posts like this. https://www.facebook.com/SupportedInOurTrials/
Friday, May 6, 2016
Pulling out tubes, etc...
If your child is capable of pulling out NG tubes/IV lines etc, you may want to invest in some "no-nos" otherwise known as pediatric arm immobilizers. Here are a few examples...
http://www.medi-kid.com/index.php?p=catalog&parent=1&pg=1
I have used the pedi-wrap brand for both arms and legs on Ellie. They do not seem too uncomfortable.
They are also good to give a good long stretch (such as overnight) for kids who have tight arms and legs. If they have a hard time sleeping with them, try putting the braces on every other night alternating on every other side.
What have you tried to keep your kids from pulling out tubes? Please comment below.
Follow our Facebook page or enter your email to the right to stay informed about upcoming posts.
https://www.facebook.com/SupportedInOurTrials/
Wednesday, May 4, 2016
Teaching Hospital and Residents/Fellows/etc...
My local children's hospital is adjacent to a medical school. Therefore, the children's hospital is a "teaching hospital". This means that when you go to appointments and the Emergency Room and are inpatient and outpatient there are LOTS and LOTS of people checking on your child. This is not always a good thing.
Let me paint you a picture. Your child is sick, you are afraid they are getting to be a little more complicated than what you feel comfortable with at home. You know from experience that if you go to your Primary Care Physician they will send you for more tests at the hospital anyway, so you skip the PCP. You decide to make the drive to the children's hospital to have them check out your child. You pack up pretty much the entire house to make the trip.
The only way to see a Dr. today is to go to the Emergency Department. It stinks, but that's the way it is. Pretty much all specialists that you would want to see are booked 3-6 months out.
The shortest I have ever had an ED visit is 2.5 hours, but typically they are over 4 hours, sometimes a lot over 4 hours. Most of the time is spent waiting, waiting and waiting. Waiting for tests to be run, waiting for Dr.'s to come by, waiting for IV fluids to go in, waiting for meds to kick in, waiting so the child can be observed, waiting for rooms to become available, etc.
So to summarize...
I know they are going to medical school. I know they need experience to become a Dr. I know they are trying to help. But here are some reasons why residents/fellows/etc are so frustrating.
Let me paint you a picture. Your child is sick, you are afraid they are getting to be a little more complicated than what you feel comfortable with at home. You know from experience that if you go to your Primary Care Physician they will send you for more tests at the hospital anyway, so you skip the PCP. You decide to make the drive to the children's hospital to have them check out your child. You pack up pretty much the entire house to make the trip.
The only way to see a Dr. today is to go to the Emergency Department. It stinks, but that's the way it is. Pretty much all specialists that you would want to see are booked 3-6 months out.
The shortest I have ever had an ED visit is 2.5 hours, but typically they are over 4 hours, sometimes a lot over 4 hours. Most of the time is spent waiting, waiting and waiting. Waiting for tests to be run, waiting for Dr.'s to come by, waiting for IV fluids to go in, waiting for meds to kick in, waiting so the child can be observed, waiting for rooms to become available, etc.
So to summarize...
- You have just changed and dropped everything your schedule to come to the hospital (not just for a few hours, but you had to look ahead for a few days and even weeks in case they are admitted inpatient)
- You are worried about your child being sick and/or wondering if they might actually die
- You had to make arrangements for all of your other children and worry about how they will cope with you being gone...yet again
- You packed up your entire house in case you end up having an extended stay at the hospital
- You are bored/tired/stressed from so much waiting
- You are thinking about all of the germs in the hospital
- The unknown is terrifying...what is wrong with my child? Will they live? How long will this hospital stay be? Are we thinking ICU or floor? Are we going to need more surgery?
I know they are going to medical school. I know they need experience to become a Dr. I know they are trying to help. But here are some reasons why residents/fellows/etc are so frustrating.
- They think they know more than you. They try to explain things that...ummm...duuhhh...I pretty much know more than you (especially regarding my child). I am not new to this game. I have been around the block more than a few times. And honestly, half the time the resident does not even know what they are talking about.
- Because they think they know more than the parents, they do not listen to you. A good experienced Dr. will compliment the parent and then ask "You know your child, what do you think is wrong?" or "You have done this before, do you have any feelings about what we should do?" or "You are a very capable parent, how can we help you?" or " You are doing a great job, how has your child responded in the past?" Residents do not compliment and they do not ask for the parents opinion or insights. Residents are trying to prove their own knowledge and worth.
- When you come to the emergency department this is how many times you have to tell what is going on (I am not exaggerating)
- Nurse or Medical Assistant when you check in (brief summary of symptoms)
- Registration (brief summary of symptoms)
- Nurse assigned to your child (I do slightly more than the brief summary...but definitely not the full story)
- Resident
- Respiratory Therapist (If RT is needed)
- Intern (Sometimes)
- Attending Physician
- Specialist (if a specialist is needed)
- Phlebotomist (not joking...they ask you what's going on...once again a brief summary)
- Other techs (CT scan, MRI, X-ray, etc...the brief summary again)
- If there is a shift change while you are in the Emergency Department start over and repeat numbers 3, 4, 5, 6, 7, 8
12. Nurse on floor
13. Tech on floor
14. Resident
15. RT
16. Intern (almost always)
17. Attending Physician
18. Specialist (if needed). If more than 1 specialist, repeat story for each specialist.
Here are some suggestions to prevent "Story Fatigue". (Yes, I just made that up...but I'm sure it is a real condition)
- Have a printed list you keep updated with the child's medications, diagnosis, allergies, surgeries and hospitalizations. Bring it with you and ask the nurse to photocopy it for you. Let the nurse use the copy to update the information she needs, then ask her to give it to the Dr. Or keep the copy and give it to the Dr. yourself when they come in. Having this list frees space in your brain to think about the critical issues at hand, saves time and prevents things from being forgotten.
- Write down everything you can remember before the attending comes in. (sometimes I will use my voice recorder on my phone while I am driving to make notes about things I want to tell the Dr. then write them down when I have a minute).
- You should write all relevant previous history relating to the current condition (ie: she has a shunt and she is acting the same way as when it failed last time)
- Recent history relating to current condition in chronological order(ie: She has been sleepy since last Sunday, she started coughing on Tuesday, and today she started needing 3 liters of oxygen)
- Any one else sick at home and symptoms
- In the ED, when the first resident type person comes in, (as long as your child is not in a really scary/bad place) tell them " I know that I will have to wait longer, but I would prefer to tell the story ONCE when they can have the "attending" present." And truly, if they are in a scary/bad place...then your child probably met "shock protocol" and the attending is already there.
- If you don't want a resident working with your child you can refuse. I do not choose this option, usually I just say I want the attending present before telling my story.
- Once you get the attending present and are ready to tell your full story for the first time...have the voice recorder ready on your phone. Record yourself telling the story (while going through all of your written notes). Keep recording when the Dr. asks some clarifying questions at the end.
- Once you get transferred to the ICU or the floor, and they start asking for the story...just pull out your phone and push "play" on your voice recorder to tell your story for each person that comes by.
What tips do you have for dealing with residents? What tips would you offer residents in their quest to becoming a "good" doctor? Please comment below.
For more stories and advice like this, please enter your email address to the right and each blogpost will be sent to you or you can "like" our FB page to get the articles in your newsfeed.
Subscribe to:
Posts (Atom)